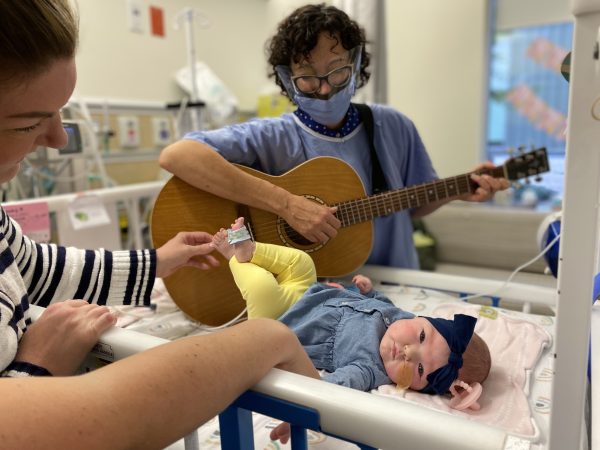
The Music Therapy Program within the Neonatal Intensive Care Unit (NICU) at BC Women’s Hospital + Health Centre began in 2018. BC Women’s Hospital is home to the largest NICU in the province of British Columbia. The 60 bed unit cares for approximately 1,700 babies each year, admitted from across BC and the Yukon Territory.
Thanks to support from Music Heals and the support of other generous donors, the NICU has been able to provide two half days of music therapy in one of the five NICU units. The unit that receives music therapy is ‘Ladybug’ – a Complex Care Unit for infants from all over BC with the most complex medical needs.
Music therapy is an effective, non-pharmacological intervention that is conducted one-on-one with the infant, and often in collaboration with other members of the health team such as physiotherapy and occupational therapy. The sessions are designed to include parents and siblings as a family-centred approach. Over 20 years of research has demonstrated the multiple positive benefits of music therapy as a non-invasive intervention for infants in the NICU, with results including increased oxygen saturation, reduced perception of pain, calming and promotion of sleep, weight gain, an increased positive auditory environment, and reduced anxiety in parents.
Demographic
BC Women’s Hospital is home to the largest NICU in the province of British Columbia. The 60 bed unit cares for approximately 1,700 babies each year, admitted from across BC and the Yukon Territory.
Age Range
28 weeks gestational age to 6 months old.
During 2021 the COVID-19 pandemic created its own unique set of mental health needs. Families were under greater stress as they coped with increased isolation both in the hospital with their infant and in caring for children at home. Music Therapy research has been shown to directly reduce anxiety in mothers of infants in the NICU. By including parents in Music Therapy sessions, singing to their infants and learning to recognize and respond to their infants’ cues they were able to gain confidence and build resilience. Music Therapy sessions in the infant’s room also could include siblings and extended family through the use of real time technology, creating those much needed links of connection, shared family time, and support.
Navigating The Ongoing COVID-19 Pandemic
COVID-19 has not caused any interruption to the NICU Music Therapy Program but it did create a greater need for services. More safety/health precautions have been put into place but the program has adapted well to creating musical connections while wearing a mask and goggles. Music Therapy has reduced the uncertainty of not seeing staff faces by providing soothing and interesting sounds to go with the covered faces. With a reduced number of visitors, family and volunteers, music therapy also has provided more one to one contact for the infants and new ways to include siblings and family in the sessions by sharing them over video or live through Zoom sessions.
There are currently 5 pods in the BCWH NICU however only 1 pod receives music therapy services. Your support will add 4 hours per week of programming and expand the service to a second pod that is currently not receiving any music therapy. This means that 5 additional NICU infants and their families could receive music therapy in their hospital rooms every week. This works out to almost 250 sessions in a year.
BC Women’s Health Foundation is committed to sustaining and expanding the music therapy program. The dream is to expand to all 5 pods in the NICU and have a full-time NICU music therapy program for all the fragile infants and their families.
“When I notice a family facing a challenging diagnosis, I think of music as a form of therapy that heals. Infants undergoing unpleasant or painful therapies are instantly calmed by music, families are provided with an extra opportunity to make meaningful memories during their infant’s hospitalization, and staff members are able to engage in an activity that is unique and developmentally supportive. The Music Therapy program has benefitted families, infants, and staff members in the neonatal intensive care unit’s complex care program. Many people turn to music for healing and having access to this service has been instrumental for our patients and families facing adversity. Everyone looks forward to our afternoons with Carol!”
– Danielle West, RN, Discharge Planning Coordinator, NICU